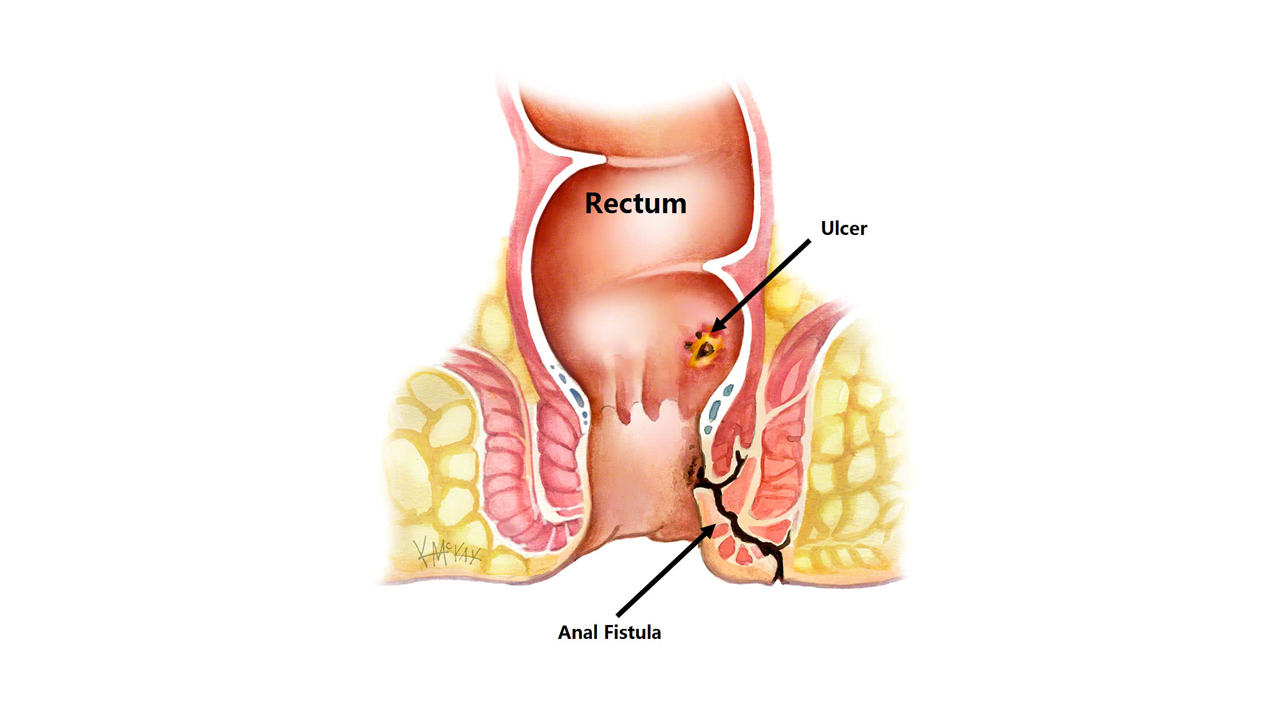
What are Anorectal conditions?
- Problems related to anus or rectums are collectively called Anorectal conditions.
- These conditions are mainly caused due to some sort of overgrowth or abnormal growth of tissues in the anus and rectum region.
- Fissures
- Piles (Hemorrhoids )
- Anal Fistula
- Prolapse
- Anal abscess
- Others-Pilonidal Sinus
HEMORRHOIDS
MIPH (MINIMAL INVASIVE PROCEDURE FOR Hemorrhoids)
(Stapler Hemorrhoidectomy)
In the past, open surgery was the only option available to surgeons when they needed to inside a patient's
body or remove or repair organ. But today minimally invasive technology is completely changing the way
doctors approach patients care. A new procedure for removing large hemorrhoids , the Stapled
Hemorrhoidectomy, is less painful and allows patients to return to work and other normal activities much
earlier than with the conventional procedure. Stapled Piles surgery is also known as PPH (Procedure for
Prolapse & Hemorrhoids ) or MIPH minimally invasive procedure for hemorrhoids.
Technique
The technique uses a stapling device and takes advantage of the fact that pain-sensing nerve Fibers are
absent higher in the anal canal. In this procedure the mucosa above the dentate line which contains part
of Piles mass, is excised & stapled with the stapler gun, thus taking care of bleeding and prolapse-
the two major components of Piles. The Piles masses are composed into a cup like cavity inside the
stapler. When fired, the titanium staples cut & seal simultaneously, thus causing minimal bleeding and
as the cutline is above the nerves, there is reduction in the Post-operation pain also. Additionally there
is no incision the perianal skin and wound in the anal mucosa is also primarily closed with
stapler.
Benefits of MIPH
 Compared to open surgery, MIPH has the following benefits:
Compared to open surgery, MIPH has the following benefits:
Day care procedure.
Shorter operation time.
Less blood loss during the operation.
Less pain after the operation.
No dressing required after the operation. Also, no hot water baths needed.
Less healing time.
The patient can get back to work on the next day of the operation.
Care to be taken after MIPH
Start Talking to Your Doctor about MIPH
Painful and prolonged traditional surgery, long healing period of four to six weeks, daily hot baths (Sitz bath) three to four times a day and embarrassment because of the location of the disease coupled with high recurrence rates of the traditional surgery contribute to patients suffering in silence rather than discussing Piles treatment with their doctor. MIPH has changed all that.
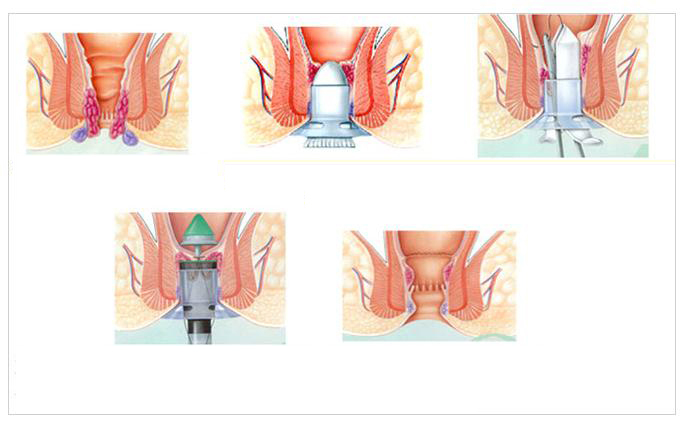
- The Stapler Technique used in MIPH
- The diagrams alongside illustrate the Stapler technique employed during MIPH.
- The picture on top shows the Piles before the operation.
- The middle two pictures show the Stapling being done.
- The bottom picture shows the effect of the Stapling.
- Facility for MIPH
- Avoid straing at stools
- Avoid constipation
- Drink enough liquids / (Water) for proper hydration
- Eat fibre rich diet (Green-leafy Vegetables)
- Exercise regularly
ANAL FISTULA
An anal fistula is defined as a small tunnel with an internal opening in the anal canal and an external opening in the skin near the anus. Anal fistulas form when an anal abscess, that's drained, doesn't heal completely.
Diagnosis
It is usually simple to locate the external opening of an anal fistula, meanwhile locating the internal
opening can be more challenging. It is important to be able to find the entire fistula for effective
treatment.
People who may have experience with recurring anal abscesses may have an anal fistula . The external
opening of the fistula is usually red, inflamed, oozes pus, and is sometimes mixed with blood.
The location of the external opening gives a clue to a fistula's likely path and sometimes the fistula can
actually be felt. However, locating its visual path often requires various tools, and often times it may
not be seen until surgery.
Tools often used in diagnosis include:
- Fistula probe. An instrument specially designed to be inserted through a fistula
- Anoscope. A small instrument to view the anal canal
- Diluted methylene blue dye. Injected into a fistula
- Fistulography. Injection of a contrast solution into a fistula and then X-raying it
- Magnetic resonance imaging
- Flexible sigmoidoscopy. A thin, flexible tube with a lighted camera inside the tip allows doctors to view the lining of the rectum and sigmoid colon as a magnified image on a television screen
- Colonoscopy. Similar to sigmoidoscopy, but with the ability to examine the entire colon or large intestine
Treatment is delicately performed to reduce the risk of affecting bowel emptying, due to the anal fistulas' proximity to the anal sphincter muscles. The best approach requires that each patient is assessed individually.
Treatment of an anal fistula is attempted with as little impact as possible on the sphincter muscles. It will often depend on the fistula's location and complexity, and the strength of the patient's sphincter muscles.
Fistulotomy
In a fistulotomy the surgeon first probes to find the fistula's internal opening. Then the tract is cut open and is scraped and its contents are flushed out.
A more complicated fistula, such as a horseshoe fistula (where the tract extends around both sides of the body and has external openings on both sides of the anus), is treated by usually laying open just the segment where the tracts join and the remainder of the tracts are removed.
The surgery may be performed in more than one stage if a large amount of muscle must be cut. The surgery may need to be repeated if the entire tract can't be found.
Seton Placement
A seton (silk string or rubber band) is used to either:
- Create scar tissue around part of the sphincter muscle before cutting it with a knife
- Allow the seton to slowly cut all the way through the muscle over the course of several weeks The seton may also aid in the drainage of the fistula.
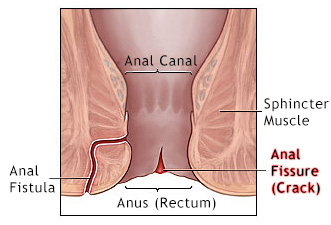
ANAL FISSURE
Anal Fissure
An anal fissure is a small tear or cut in the skin that lines the anus. Fissures typically cause pain and
often bleed. Fissures are quite common, but are often confused with other causes of pain and bleeding,
such as hemorrhoids.
Symptoms of an Anal Fissure
The typical symptoms of an anal fissure are pain during or after defecation and bleeding. Patients may try
to avoid defecation because of the pain.
Causes of Anal Fissure
Trauma: anything that can cut or irritate the inner lining of the anus can cause a fissure. A hard, dry bowel movement is typically responsible for a fissure. Other causes of a fissure include diarrhea or inflammatory conditions of the anal area. Anal fissures may be acute (recent onset) or chronic (present for a long time or recurring frequently). Chronic fissures often have a small external lump associated with the tear called a sentinel pile or skin tag.
TreatmentOften treating one’s constipation or diarrhea can cure a fissure. An acute fissure is typically managed with non-operative treatments and over 90% will heal without surgery. A high fiber diet, bulking agents (fiber supplements), stool softeners, and plenty of fluids help relieve constipation, promote soft bowel movements, and aide in the healing process. Increased dietary fiber may also help to improve diarrhea. Warm baths for 10-20 minutes several times each day are soothing and promote relaxation of the anal muscles, which can also help healing. Occasionally, special medications may be recommended. A chronic fissure may require additional treatment.
Will the problem return
Fissures can recur easily, and it is quite common for a healed fissure to recur after a hard bowel movement. Even after the pain and bleeding has disappeared one should continue to aim for good bowel habits and adhere to a high fiber diet or fiber supplement regimen. If the problem returns without an obvious cause, further assessment may be needed.
What can be done if a fissure doesn’t heal?
A fissure that fails to respond to treatment should be re-examined. Persistent hard or loose bowel movements, scarring, or spasm of the internal anal sphincter muscle all contribute to delayed healing. Other medical problems such as inflammatory bowel disease, infections, or anal growths (skin tumors) can cause fissure-like symptoms, and patients suffering from persistent anal pain should be examined to exclude these conditions.
Surgery for Anal Fissure
Surgery is a highly effective treatment for a fissure and recurrence rates after surgery are low. Surgery usually consists of a small operation to cut a portion of the internal anal sphincter muscle (a lateral internal sphincterotomy). This helps the fissure heal and decreases pain and spasm.
If a sentinel pile is present, it too may be removed to promote healing of the fissure. A sphincterotomy rarely interferes with one’s ability to control bowel movements and is most commonly performed as a short outpatient procedure.
Pilonidal Sinus
A pilonidal sinus is a small hole or "tunnel" in the skin. It usually develops in the cleft of the
buttocks where the buttocks separate.More than one hole may develop, and often these are linked by tunnels
under the skin.
Most people associate the word sinus with the nose, but sinuses can occur anywhere in the body. Sinus is
simply a medical term for a channel or cavity.A pilonidal sinus will not usually cause any noticeable
symptoms unless it becomes infected. This can cause a pus-filled abscess to develop. Signs that you may
have an infection include pain, redness and swelling in the affected area.
Treating a pilonidal sinus
Treatment may not be necessary for a pilonidal sinus if it's not infected.
It's important to keep the area as clean and dry as possible. Removing hair from the area is also
advisable, usually by shaving or using hair removal creams. This should reduce the risk of an
infection.
If your pilonidal sinus does become infected, surgery is likely to be recommended.